Bariatric surgery is one of the most effective tools we have for treating severe obesity. It can help people lose 60–80 percent of their excess weight and improve or resolve conditions like diabetes and hypertension. But surgery doesn’t cure obesity. Weight loss typically peaks 12–18 months after surgery, and some regain is normal as your body adapts. Studies show that as many as 76 % of patients experience some weight recurrence within six years. In one long‑term study, people had regained roughly 31 % of the weight they initially lost after six years. Another report found that about one‑third of patients gained more than 25 % of their original weight within two to five years, and more than 40 % regained weight within 10 years.
These numbers can feel discouraging, but they don’t mean the surgery failed or that you have failed. Obesity is a chronic, relapsing disease, and long‑term success requires ongoing lifestyle and psychological support. Understanding why weight regain happens—and how to respond early—can help you stay on track.
What Is Weight Recurrence?
After surgery you will lose weight rapidly, then reach a steady “nadir” or lowest weight. Weight recurrence refers to weight gained after reaching your lowest post‑surgery weight. Small gains of a few kilograms are common and reflect normal metabolic adjustment. Larger gains can lead to the return of obesity‑related health problems and should prompt a reassessment with your healthcare team.
Why Weight Regain Happens
Loss of healthy habits, grazing and high‑calorie foods
Early on, most people are diligent with portion sizes, eat balanced meals and avoid trigger foods. Over time, it can be hard to maintain new habits. You may start to tolerate a wider variety of foods, eat larger portions or skip exercise. Cleveland Clinic dietitian Dr Lillian Craggs‑Dino notes that weight recurrence often boils down to behavioural factors such as binge eating, eating when you feel full, eating continuously throughout the day and choosing high‑fat, high‑calorie foods. After surgery your metabolism slows, so eating the same number of calories you did at 300 pounds will cause weight gain at 150 pounds.
Decreased physical activity and metabolic adaptation
Weight loss following bariatric surgery reduces your resting metabolic rate. Without regular activity, the calories you burn each day drop significantly. Many patients exercise consistently in the first year but then gradually cut back. Dr Craggs‑Dino recommends aiming for 300–400 minutes of exercise per week, including both cardiovascular and strength training. When exercise declines and sedentary habits creep in, even small extra calories can lead to regain.
Psychological and emotional factors
Bariatric surgery changes your digestive system, but it doesn’t remove the emotional drivers of eating. A Cleveland Clinic study found that patients who scored high on measures of emotional/internalizing dysfunction (depression, anxiety and mood problems) and impulsivity were more likely to experience weight recurrence. The researchers noted that depression, anxiety, emotional distress and aggression were all associated with more weight gain, while positive emotions and low impulsivity appeared to protect against it. CommonSpirit Health points out that emotional eating is a learned behaviour—people eat when bored, lonely or sad—and that depression and anxiety make adherence to postoperative instructions more challenging, which can lead to weight regain. Addressing mental health and developing healthy coping skills are therefore essential.
Anatomical and surgical factors
Although modern bariatric procedures are designed to be durable, anatomical changes can contribute to weight regain in some patients. Over time the gastric pouch or sleeve may stretch, increasing capacity and appetite. Murrieta Valley Surgery Associates notes that pouch dilatation, stretching of the stoma (the connection between the stomach and intestine), problems with adjustable bands, or a gastric‑gastric fistula can all reduce restriction and lead to more eating. In rare cases, medical circumstances such as pregnancy, thyroid or adrenal problems or new medications can cause weight gain.
Lack of follow‑up and support
Regular follow‑up visits and support from your bariatric team play a major role in long‑term success. Murrieta’s clinicians observe that patients who attend routine clinic visits tend to gain less weight than those who skip follow‑ups. Cleveland Clinic likewise emphasises staying connected with your team; they can offer new strategies, additional support or medications if weight begins to climb. Without ongoing accountability and guidance, it’s easy to revert to old behaviours.
How to Prevent Weight Regain
Follow your nutrition plan
Nutrition is the foundation of long‑term success. Dr Craggs‑Dino advises centering your meals on lean proteins, vegetables, fruits and whole grains. Portion control matters—your bariatric procedure helps you feel full on less food, but only if you stick to smaller servings. Limit added sugars and processed foods, and avoid grazing; snacking all day keeps you from feeling full and adds extra calories. If you struggle to meet protein goals, work with a dietitian to develop meal plans and track your intake.
Stay active
Exercise maintains muscle mass, boosts metabolism and reduces stress. Cleveland Clinic recommends 300–400 minutes of weekly exercise that combines cardio and strength training. If that sounds daunting, start where you are and build up gradually—every bit helps. Choose activities you enjoy (walking, swimming, dancing, cycling) so you’ll stick with them.
Prioritise mental and emotional health
Monitor your mood and look for patterns between emotions and eating. Keep a food journal to identify triggers, practise mindful eating and ask yourself whether you’re truly hungry before snacking. Seek support from a therapist or support group if you struggle with depression, anxiety or emotional eating. The Cleveland Clinic study underscores that addressing depression, anxiety and impulsivity can help prevent weight recurrence.
Stay connected with your bariatric team
Don’t wait until weight gain becomes significant. Schedule regular check‑ins with your surgeon, dietitian and primary care provider. They can evaluate potential anatomical issues (such as pouch or stoma dilation) and adjust your plan. Cleveland Clinic notes that early intervention is easier and your team may recommend medications or revision procedures if lifestyle changes aren’t enough.
When to Seek Help
If you regain 10 % or more of the weight you lost, or if you notice new symptoms such as reflux, vomiting, persistent hunger or changes in eating capacity, contact your bariatric team. Early assessment can identify correctable issues and prevent further gain. Weight recurrence may indicate an anatomical change or a need for more intensive support.
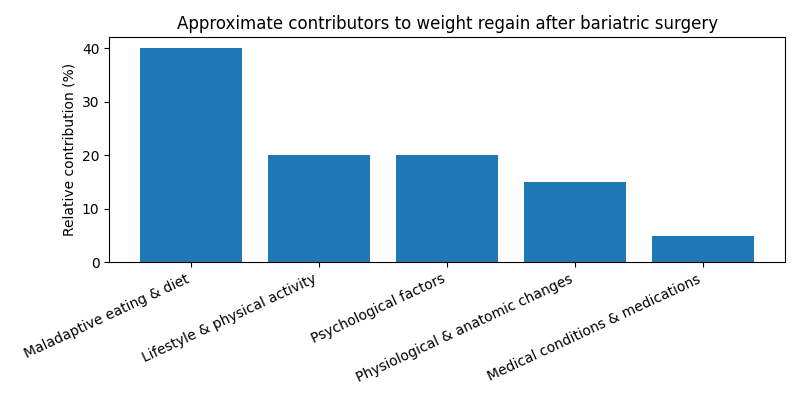
Visualising the Causes of Weight Regain
The bar chart below illustrates the relative contributions of behavioural, lifestyle, psychological, anatomical and medical factors to weight regain. While the exact percentages vary across studies, it underscores that behavioural and lifestyle factors play the largest role.
Final Thoughts
Weight regain after bariatric surgery is common and manageable. It does not mean the surgery failed or that you’ve done something wrong. Understanding the root causes—whether it’s slipping back into old habits, exercising less, emotional eating, anatomical changes or life events—can help you take proactive steps. Focus on protein‑rich, whole‑food nutrition, consistent physical activity, emotional self‑care and regular follow‑up with your medical team.
At Novara Academy, we address weight recurrence through our Life After: Next Chapter and Evolve: Continuing the Journey programs, offering personalised nutrition coaching, mindset work and community support. If you notice weight creeping back, don’t wait—reach out to your team, lean on your community and remember that long‑term success is built on consistent, compassionate self‑care. Your transformation is an ongoing journey, and you’re not alone.

