Many people still think of weight‑loss surgery as a desperate measure, something you do only when every diet and medication has failed. A national survey found that 79 percent of Americans believe bariatric surgery should be pursued only as a last resort and 60 percent think it’s a shortcut for losing weight. Despite strong evidence and improvements in safety, only about 1 percent of people who are clinically eligible ever undergo surgery. These misperceptions delay treatment and cost lives.
This article challenges the “last resort” mindset. Obesity is a chronic disease, not a personal failing. Bariatric surgery isn’t a quick fix, but it is the most effective and durable treatment we have for severe obesity. When used at the right time and paired with lifestyle and psychological support, it can prevent comorbidities, improve quality of life and extend lifespan. Below we explore why waiting can be harmful, why early intervention makes sense and how to reframe your decision.
Why People Still See Surgery as a Last Resort
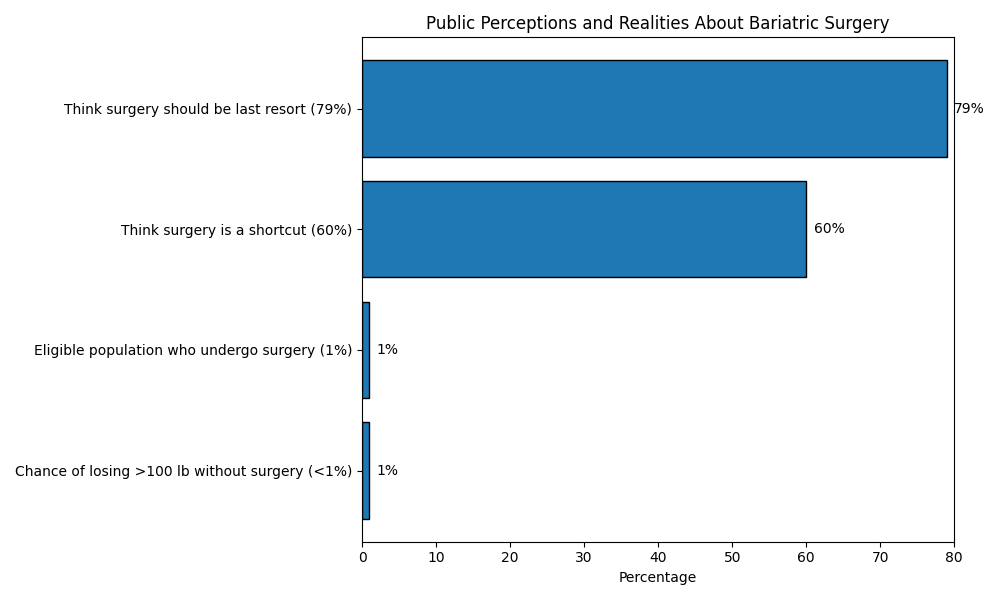
Stigma and misinformation keep many people from considering bariatric surgery. In the Orlando Health/Ipsos survey mentioned above, nearly four out of five Americans said weight‑loss surgery should only be used after all other options have failed. Sixty percent even labeled it a “shortcut,” despite the fact that patients must commit to lifelong diet, exercise and follow‑up. These attitudes contribute to under‑utilization; one survey found that only 1 percent of people who meet the criteria for metabolic and bariatric surgery (MBS) actually have it. The chart below illustrates the gulf between public perception and reality.
Obesity Is a Chronic Disease, Not a Lifestyle Choice
Modern medicine recognises obesity as a complex, chronic disease influenced by genetics, hormones, metabolism and environment. It is not a sign of laziness or a lack of willpower. As Dr Ali Zarrouk’s practice explains, obesity results from changes in hormones, metabolism and brain chemistry, and bariatric surgery should not be seen as a last resort but as an effective treatment option offered early enough to make a real difference. The same article notes that dieting alone often fails because the body defends its weight by lowering metabolism and increasing hunger hormones. Surgery changes gut hormones such as ghrelin and GLP‑1, helping reset the body’s weight‑regulation system.
The Grand Health Partners team echoes this message. They stress that bariatric surgery is not a last‑ditch effort for people who “failed” at dieting but a well‑established medical treatment for a chronic disease. Long‑term studies show surgery is more effective than diet and exercise alone in treating severe obesity and improving survival. Recognised bodies such as the American Society for Metabolic and Bariatric Surgery (ASMBS) and the National Institutes of Health call surgery the gold standard for treating severe obesity.
Evidence: Surgery Works – and Works Best When Used Early
Long‑term weight loss is nearly impossible without surgery
The Cedars‑Sinai health system tackles one of the biggest myths head‑on. They cite a National Institutes of Health expert panel showing that for people who are severely obese, long‑term weight loss is nearly impossible without surgery. Intervening within five years of developing a weight‑related condition (such as diabetes) leads to better long‑term outcomes. Dr Sandhu, one of their bariatric surgeons, notes that one of the most common comments he hears from patients after surgery is: “I wish I’d done the surgery sooner”.
Early intervention is safer and more effective
An international panel of experts convened by the ASMBS and the International Federation for the Surgery of Obesity recommends expanding access to metabolic and bariatric surgery and lowering BMI thresholds because obesity is a progressive disease. Dr Ali Aminian of Cleveland Clinic explains that “it is always safer to intervene earlier… rather than waiting until patients gain more weight and develop severe disease”. He likens it to treating heart disease or cancer early, noting that surgery shouldn’t be viewed as the last resort reserved only for extremely high BMI cases.
Diet and exercise rarely succeed in severe obesity
Dr Katherine Meister of TriHealth underscores why surgery is often necessary: the chances of a patient more than 100 lb overweight losing that weight without surgery are less than 1 percent. She emphasises that obesity is as serious as heart disease or cancer and that intervening earlier improves survival and quality of life. Surgery is just one piece of the puzzle, but for many patients it’s the critical piece that unlocks success.
Surgery is proven safe and durable
Modern procedures such as sleeve gastrectomy and gastric bypass are performed laparoscopically, with mortality rates around 0.2 %—similar to gallbladder surgery. A systematic review summarised by the ASMBS found that bariatric surgery produces greater, sustained weight loss than lifestyle interventions or GLP‑1 receptor agonist medications and is considered the most effective and durable treatment for obesity. Patients typically lose 20–40 % of their body weight and sustain it for decades.
Why Waiting Hurts: Risks of Delaying Surgery
Progressive disease and rising complications
Obesity is progressive. Every year a person lives with severe obesity raises their risk of developing type 2 diabetes, hypertension, fatty liver disease, joint damage, sleep apnea and fertility issues. Dr Aminian cautions that for obesity, as with heart disease or cancer, earlier treatment is safer and more effective. Waiting until BMI is extremely high makes surgery more technically challenging and increases health risks.
Lost years of health and happiness
Sterling Surgicare points out that acting early means more years with improved energy, mobility and freedom from chronic disease. Early surgery prevents irreversible damage and allows younger bodies to heal and adapt faster. It also gives people time to build confidence and reshape their self‑image, turning surgery into a turning point rather than a last resort.
Missed opportunity to prevent comorbidities
The Lancet Diabetes & Endocrinology editorial, summarised by the North Queensland Obesity Surgery Centre, warns that when bariatric surgery is reserved for severe obesity with progressive comorbidities, we miss the opportunity to prevent those conditions. The authors argue that surgery should be available as an option when appropriate—not only when all other options have been eliminated. Using surgery only as a final resort “will miss the opportunity for preventing comorbid diseases and complications of obesity”.
Bariatric Surgery Is Not a Shortcut
Contrary to myth, surgery is not an “easy way out.” The Trinity Health Michigan bariatric program notes that while rapid and significant weight loss can be achieved, surgery requires hard work and commitment; it should be considered a healthy option and not a last resort. Patients must change eating and exercise habits and attend follow‑up care to succeed. Grand Health Partners reinforces that obesity is a complex disease influenced by genetics and hormones; surgery is a powerful tool that resets metabolic pathways and helps build a healthier life, but long‑term success depends on ongoing support.
Dr Meister emphasises a multidisciplinary approach that includes surgeons, dietitians, psychologists, exercise physiologists and primary care physicians. Surgery is one piece of the puzzle; lifestyle changes, mental health support and long‑term follow‑up complete the picture.
Reframing the Decision
Seeing bariatric surgery as a last resort doesn’t serve patients or public health. Obesity is a disease, and we don’t wait until cancer is advanced before offering chemotherapy or postpone insulin until diabetes causes organ damage. As several experts note, we should treat obesity early to prevent complications.
Reframing the decision means understanding that:
- Surgery is a proven, evidence‑based treatment for severe obesity, not a sign of failure.
- Early intervention is safer and yields better outcomes—medically, surgically and psychologically.
- Waiting can cause irreversible damage, limit surgical options and shorten lifespan.
- Lifestyle changes and support are still essential; surgery works best when paired with nutrition counselling, exercise, behavioural therapy and long‑term follow‑up.
Your Next Step
If you’re living with obesity, you deserve timely, respectful care based on science—not outdated beliefs. Talk with a qualified bariatric surgeon about your options, even if you haven’t reached an extremely high BMI. The Novara Academy Pre‑Op programme helps you prepare physically and mentally for weight‑loss surgery, while Life After and Evolve offer ongoing support to help you thrive post‑surgery. You don’t have to wait until you’ve exhausted every other option. By acting sooner, you can reclaim your health, reduce complications and gain years of vibrant living.

