Bariatric surgery can be life‑changing, but it’s still major surgery. Understanding potential risks and side effects helps you make an informed decision and manage your recovery. The good news? Metabolic/bariatric surgery is safer than many common operations — the American Society for Metabolic and Bariatric Surgery reports a 0.1 % risk of death and roughly 4 % chance of major complications. In other words, for most people with severe obesity the benefits outweigh the risks. Let’s examine the possible complications so you can approach your journey with eyes wide open.
Short‑Term Surgical Risks
All abdominal surgeries carry certain risks. Bariatric procedures are usually performed laparoscopically, which reduces risk, but complications can still happen:
- Bleeding, infection and blood clots. These are common risks for any surgery. Your surgical team will use antibiotics, blood‑thinning medications and early mobilization to reduce them.
- Anesthesia reactions. Some people experience adverse reactions to general anesthesia; anesthesiologists monitor you closely during surgery.
- Leaks at surgical connections. In procedures like gastric bypass, surgeons connect two parts of your digestive tract. Rarely, the connection may not seal completely, causing an anastomotic leak. This serious complication can lead to infection and sepsis. Fortunately, leaks occur in roughly 5 % of anastomosis surgeries and are most common in complex operations. Surgeons perform leak tests during surgery and monitor you after discharge.
- Small bowel obstruction or hernias. Scar tissue can sometimes block your intestines or create a hernia; prompt medical evaluation is needed if you develop severe abdominal pain or vomiting.
Digestive System Side Effects
Dumping Syndrome (Rapid Gastric Emptying)
After gastric bypass or other stomach surgeries, you may experience dumping syndrome — when food empties too quickly into your small intestine. Up to 20 % – 50 % of people who have had stomach surgery develop symptoms. Rapid gastric emptying can cause nausea, abdominal cramps, diarrhea and blood sugar swings. Early dumping happens within 30 minutes of eating; late dumping occurs 2–3 hours after a meal and may cause shakiness and faintness. Dumping syndrome is uncomfortable but not usually dangerous; symptoms improve over time and are managed by eating small, low‑sugar meals and avoiding liquids at meals.
Malabsorption and Malnutrition
Surgeries that bypass or remove sections of the small intestine can cause malabsorption — difficulty absorbing nutrients. Malabsorption leads to diarrhea and nutrient deficiencies. Over time, deficiencies in protein, fats, vitamins and minerals can cause weight loss, muscle wasting, weakened immunity, bone loss, skin and hair changes. Because of these risks, you’ll take daily multivitamins and mineral supplements for life and have regular blood tests to monitor levels.
Bile Reflux
When bile flows backward into your stomach or esophagus, it’s called bile reflux. This can happen when surgical changes or a weak pyloric valve allow digestive juices to backwash. Bile is harsh on stomach and esophageal linings and may cause burning stomach pain, nausea and greenish vomiting. Bile reflux is uncommon but occurs more often after stomach surgery. Treatment includes medications to promote motility and acid suppression and, rarely, revisional surgery.
Gallstones
Rapid weight loss increases your risk of gallstones — hardened pieces of bile that can block your bile ducts. About 10 % of adults have gallstones; roughly 20 % of those experience symptoms. Rapid weight loss after bariatric surgery and changes in bile composition can cause stones to form. Symptoms include upper abdominal pain, nausea, fever and jaundice. Your provider may recommend gallbladder removal during bariatric surgery if you have gallstones or prescribe medications to reduce stone formation.
Kidney Stones
Changes in digestion can also increase your risk of kidney stones. Malabsorptive procedures (such as gastric bypass) lead to fat binding calcium in the intestine, leaving excess oxalate to be absorbed and excreted in urine. Dehydration from diarrhea further concentrates urine. Over time, calcium oxalate crystals can form stones. Staying hydrated (at least 2.5 liters of fluid daily), limiting animal protein and salt, and increasing citrate (from lemon or lime) can help prevent stones.
Anastomotic Leaks
As mentioned above, anastomotic leaks occur when the connection between two sections of the digestive tract doesn’t seal. Leaks can cause peritonitis and sepsis. Risk factors include smoking, malnutrition, immunosuppressant use, long operation times and certain anatomical locations. Surgeons check for leaks during and after surgery; symptoms include severe abdominal pain, fever and rapid heart rate.
Bowel Obstruction, Ulcers and Other Long‑Term Complications
Long‑term complications of gastric bypass may include bowel obstruction, hernia, ulcers, perforation and vomiting. Ulcers at the connection site (marginal ulcers) occur in a small percentage of patients and may be linked to smoking, non‑steroidal anti‑inflammatory drug (NSAID) use or Helicobacter pylori infection. Hypoglycemia (low blood sugar) is a rare complication usually related to dumping syndrome; improved insulin sensitivity after surgery can trigger episodes. Hair thinning, dry skin, cold sensitivity, fatigue and mood changes are common during rapid weight loss but usually improve as your weight stabilizes.
Psychological and Social Considerations
Surgery doesn’t just affect your body — it can impact your mental health and relationships. In the months following bariatric surgery, some people experience depression, alcohol or substance abuse, changes in social relationships, hair loss and sagging skin. Women may become more fertile after significant weight loss, so pregnancy should be avoided for 12–18 months. It’s essential to work with a mental health professional and support group to navigate emotional changes and prevent transfer addictions.
Risk vs. Benefit
Despite these potential complications, bariatric surgery remains one of the most effective and long‑lasting treatments for severe obesity. It improves or resolves conditions like type 2 diabetes, sleep apnea, hypertension and heart disease. Studies show that bariatric surgery can reduce your risk of premature death by 30 %–50 %. Major complications occur in roughly 4 % of cases and the risk of death is around 0.1 %, comparable to gallbladder removal or appendectomy. Choosing an experienced surgical team and following their instructions significantly reduces risks.
Chart: Selected Complications and Their Frequency
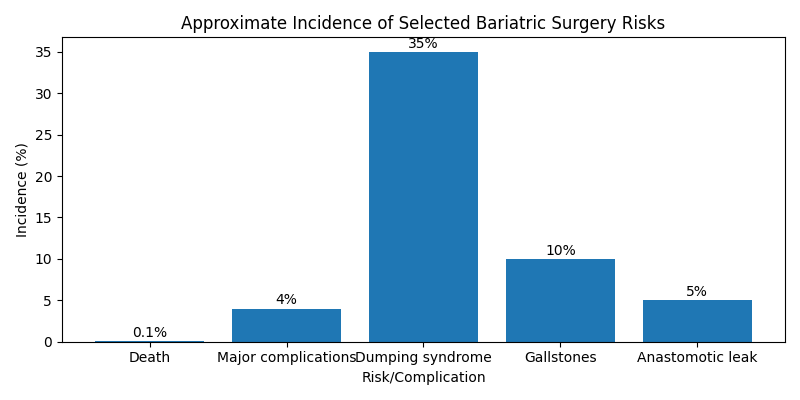
Preventing and Managing Complications
While you can’t eliminate all risks, you can reduce them:
- Choose an experienced bariatric team. Surgeons and programs accredited by the American College of Surgeons and ASMBS have lower complication rates.
- Follow presurgical and postsurgical instructions. Quit smoking, manage chronic conditions and adhere to dietary and activity guidelines.
- Attend all follow‑up appointments. Regular check‑ups allow your team to monitor healing, detect complications early and adjust medications or supplements.
- Take prescribed vitamins and minerals. Lifelong supplementation prevents malnutrition and nutrient deficiencies.
- Eat slowly and mindfully. Small, nutrient‑dense meals reduce dumping syndrome and minimize strain on your digestive system.
- Stay hydrated. Drinking at least 2.5 liters of water daily helps prevent kidney stones and supports overall digestion. Avoid alcohol and sugary beverages.
- Exercise and maintain mental health. Physical activity improves recovery; counseling and support groups can help you navigate emotional challenges.
Conclusion
Bariatric surgery carries risks, but most are manageable and far outweighed by the potential health benefits. Understanding these side effects empowers you to take proactive steps for a safe recovery. With the right support — from your healthcare team, family, and programs like Novara Academy’s Life After and Evolve — you can minimize complications and achieve lasting results. Always discuss your personal risk factors with your surgeon and remember: informed preparation is your best defense.

