Bariatric surgery is a powerful tool for weight loss, but it isn’t a magic wand.
It reduces stomach size and changes digestion, yet long‑term success depends on your commitment to new habits.
After the initial excitement fades, many patients are surprised by how much there is to learn about eating, supplementation, exercise and emotional wellness.
This guide answers the questions most surgeons never fully explain and prepares you for the realities of life after surgery.
The Healing Diet: What to Expect
Immediately after bariatric surgery, your digestive system needs time to heal.
Doctors and dietitians use a phased approach so you can gradually reintroduce food without stressing your stomach.
According to the Mayo Clinic, patients advance through clear liquids, pureed foods, soft foods and finally solid foods over roughly 6–8 weeks.
Key guidelines include drinking at least 64 ounces (1.9 litres) of fluid per day, sipping between meals, eating slowly, prioritising protein and choosing low‑fat, low‑sugar foods.
The table below summarises the typical timeline:
| Phase | Approx. timeline | What you can consume | Tips |
|---|---|---|---|
| Clear liquids | Days 0–7 | Broth, unsweetened juice, decaffeinated tea/coffee, skim milk and sugar‑free gelatin | Sip slowly between meals; aim for 64 oz of fluid but avoid drinking 30 minutes before or after meals |
| Pureed/blended foods | Week 2–3 | Strained or mashed foods (lean meats, cottage cheese, scrambled eggs, cooked cereal, soft fruit and vegetables) blended with water or skim milk | Eat 3–6 small meals of 4–6 tablespoons; take 30 minutes per meal and puree thoroughly |
| Soft foods | Week 3–6 | Soft, tender foods such as ground meat, flaked fish, eggs, cottage cheese, cooked cereals, rice and canned fruit | Continue eating slowly; chew each bite until it reaches a pureed consistency before swallowing |
| Solid foods | Week 8 and beyond | Gradually reintroduce firmer foods in small portions | Eat three small meals per day (1–1.5 cups each); avoid foods that can cause blockages or dumping syndrome |
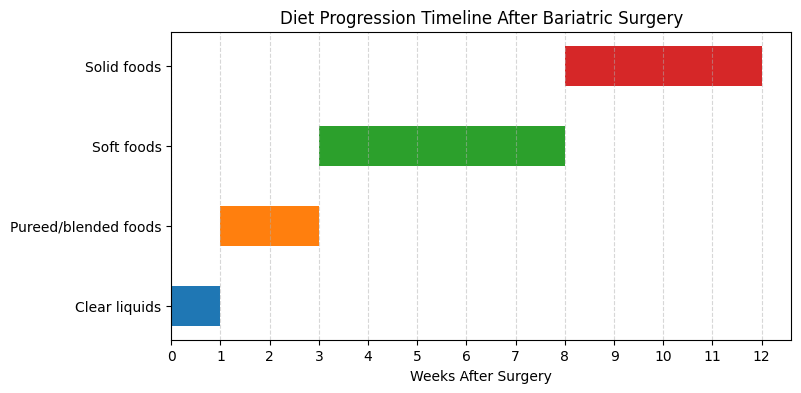
Visual Timeline
To help visualise your diet progression, the graphic below shows when each phase typically begins and ends.
Note: your surgeon or dietitian may adjust this schedule based on your healing.
Take Your Vitamins & Supplements for Life
Bariatric surgery permanently alters the way your body absorbs nutrients.
The American Society for Metabolic and Bariatric Surgery (ASMBS) stresses that lifelong vitamin and mineral supplementation is mandatory.
Most patients require a multivitamin, extra vitamin B12, calcium, vitamin D and iron to prevent deficiencies.
Skipping supplements can lead to anaemia, bone loss, neurological problems and other serious health issues.
Work with your healthcare team to choose bariatric‑specific formulations and have your blood levels checked regularly.
Move Your Body
Regular physical activity is crucial for maintaining weight loss and overall health.
ASMBS recommends starting with gentle walking soon after surgery and gradually working up to 30 minutes of moderate exercise daily.
Low‑impact activities like walking, swimming, cycling or using an elliptical machine are ideal while you heal.
Strength training can begin later (once cleared by your surgeon) to help preserve muscle mass.
Remember: exercise not only burns calories, it boosts mood, improves sleep and supports long‑term weight maintenance.
Medication Adjustments
Weight‑loss surgery often leads to improved blood pressure, blood sugar and cholesterol.
Many medications may need to be stopped, reduced or converted into liquid or chewable forms after surgery.
Never make changes yourself—always work with your prescribing doctors.
Some patients will still need anti‑acid medication temporarily, and you should avoid non‑steroidal anti‑inflammatory drugs (NSAIDs) because they can increase ulcer risk.
Alcohol, Smoking & Pregnancy
Your body absorbs alcohol much faster after bariatric surgery.
ASMBS warns that blood alcohol levels rise more quickly and fall more slowly, increasing the risk of intoxication and alcohol misuse.
If you drink, do so sparingly and never on an empty stomach.
Smoking or vaping impedes healing and increases the risk of ulcers and other complications; patients are urged to quit completely.
Women should avoid pregnancy for 12–18 months post‑surgery to allow weight and nutrient levels to stabilise.
Weight loss can improve fertility, so effective contraception is essential until your doctor gives the all‑clear.
Long‑Term Follow‑Up
Obesity is a chronic disease, and surgery is only the beginning.
Regular follow‑up visits—every few months during the first year, then annually—help monitor weight, adjust medications and catch nutrient deficiencies early.
Staying connected to your bariatric team provides accountability and access to resources like support groups, dietitians and mental health professionals.
Common Post‑Op Concerns
Hair Loss
Many patients notice increased hair shedding around 3–4 months after surgery.
Healthline notes that rapid weight loss, surgical stress and nutrient deficiencies (especially low zinc, iron, folate and ferritin) can cause temporary hair loss known as telogen effluvium.
This condition doesn’t usually lead to bald spots; hair growth typically resumes within about six months【982481212631039†L391-L494】.
To minimise hair loss:
- Follow your nutrition plan: meet your daily protein goals and take supplements as prescribed.
- Avoid excessive supplements: too much vitamin A, vitamin E or selenium can worsen hair loss.
- See your doctor if hair loss persists beyond six months; it may signal a nutrient deficiency.
Dumping Syndrome
Dumping syndrome occurs when food empties from your stomach into the small intestine too quickly.
Cleveland Clinic explains that it’s common after gastric bypass or other stomach surgeries and affects 20–50 % of patients.
Early dumping syndrome triggers nausea, abdominal cramps, bloating, diarrhea and dizziness within 10–30 minutes after eating.
Late dumping (two to three hours later) can cause weakness, shakiness, rapid heartbeat and low blood sugar.
Fortunately dumping syndrome is rarely serious and usually improves over time.
You can reduce symptoms by eating smaller meals, avoiding high‑fat and high‑sugar foods, chewing thoroughly and drinking liquids between meals rather than with meals.
Gallstones
Rapid weight loss increases the risk of gallstones.
The Obesity Action Coalition reports that 25–30 % of bariatric patients may develop symptomatic gallstone disease within the first year after surgery.
Some surgeons advocate removing the gallbladder during bariatric surgery, but this is debated because it exposes many patients to unnecessary risk.
Discuss your personal risk and prevention strategies (such as medications that dissolve gallstones) with your surgeon.
Emotional & Social Changes
Bariatric surgery isn’t just a physical transformation—it changes how you feel about yourself and how others relate to you.
Brown University health experts note that patients often enter surgery with feelings of shame and low self‑esteem; afterwards they may struggle with body image, relationships and lifestyle adjustments.
Important strategies include:
- Build a support network: surround yourself with people who encourage healthy habits and join a bariatric support group.
- Celebrate non‑scale victories: pay attention to improvements in mobility, energy, sleep and confidence rather than just the number on the scale.
- Develop healthy coping mechanisms: learn to manage stress without turning to food; exercise, journaling and therapy can help.
Mental health support is vital; don’t hesitate to seek counselling to help navigate identity shifts and relationship dynamics.
Final Thoughts & Next Steps
Life after bariatric surgery can be challenging, but it’s also incredibly rewarding.
By following your post‑surgery diet, taking your supplements, staying active, managing complications and nurturing your emotional health, you’ll set yourself up for long‑term success.
Remember, you’re not alone on this journey.
Novara Academy’s Life After: Next Chapter program offers guidance, accountability and community during the first year after surgery, while Evolve helps graduates continue their transformation.
If you’re ready for expert support every step of the way, explore our programs and join a community that understands what you’re going through.

