Bariatric surgery is more than a weight‑loss procedure—it’s a metabolic intervention that can reset your physiology and open the door to a healthier life. At Novara Academy, we support people before and after surgery with education, coaching and community. This post breaks down the basics so you can decide if bariatric surgery is right for you.
Disclaimer: This guide is for educational purposes only and does not replace medical advice. Always consult a qualified bariatric surgeon and your health‑care team before making decisions.
What is bariatric surgery?
Bariatric surgery refers to several operations that alter your digestive system to treat severe obesity. By reducing the size of the stomach and sometimes rerouting the intestines, these procedures limit how much you can eat and change how your body absorbs and processes food. They’re not “the easy way out;” bariatric surgery is a tool that requires lifelong commitment to new eating habits, physical activity and follow‑up care.
Who is bariatric surgery for?
Candidates usually have a body mass index (BMI) of 40 or higher, or BMI ≥ 35 with serious obesity‑related health conditions like type 2 diabetes, high blood pressure or sleep apnea. Some guidelines now allow surgery for patients with BMI ≥ 30 if their diabetes is uncontrolled. A thorough medical evaluation and psychological assessment are essential to determine whether surgery is appropriate and to identify any challenges ahead.
Tip: In our Pre‑Op: Preparing for Next Chapter program, we help you gather medical records, understand insurance requirements and prepare mentally for the journey.
Types of bariatric surgery
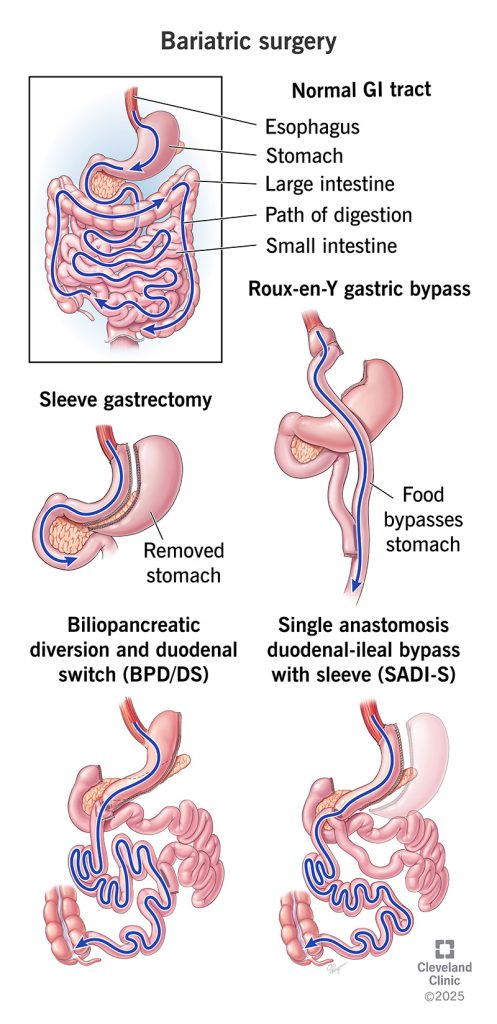
Bariatric surgery isn’t one‑size‑fits‑all. The most common procedures include:
Sleeve gastrectomy (sleeve)
Surgeons remove about 80 % of the stomach, leaving a narrow sleeve or “banana‑shaped” pouch. This restricts portion sizes and reduces levels of the hunger hormone ghrelin. Weight loss is significant but tends to be slightly slower than with gastric bypass.
Roux‑en‑Y gastric bypass
The stomach is divided to create a small pouch, which is then connected directly to the middle portion of the small intestine, bypassing the rest of the stomach and the first part of the intestines. This procedure produces more rapid weight loss and stronger effects on hormones and metabolism, but it carries a higher risk of nutritional deficiencies.
Biliopancreatic diversion with duodenal switch (BPD/DS)
This operation combines a sleeve gastrectomy with a more extensive intestinal bypass. It can lead to dramatic weight loss and improvements in diabetes but requires rigorous vitamin supplementation to prevent severe malabsorption.
Single anastomosis duodeno‑ileal bypass with sleeve (SADI‑S)
SADI‑S is a newer variation of the duodenal switch that bypasses about half of the small intestine. It offers significant weight loss with slightly less malabsorption than the traditional duodenal switch. The choice between procedures depends on your BMI, health conditions and preferences—discuss these factors with your surgeon.
Benefits of bariatric surgery
- Durable weight loss: Bariatric surgery is the only obesity treatment proven to produce substantial, long‑term weight loss. Many patients lose 50–70 % of their excess weight with sleeve gastrectomy and 60–80 % with gastric bypass.
- Improved health: Surgery often leads to remission or dramatic improvement of type 2 diabetes, hypertension, high cholesterol and sleep apnea. Reduced hunger hormones and metabolic changes make it easier to maintain weight.
- Enhanced quality of life: Patients frequently report more energy, less joint pain, increased mobility and better mood. Many people are able to reduce or discontinue medications.
Risks and side effects
Like any surgery, bariatric procedures carry risks. Potential complications include bleeding, infection, blood clots and leaks at the surgical connections. Long‑term side effects may involve dumping syndrome (nausea, dizziness and diarrhea after eating sugary foods), malabsorption, vitamin deficiencies and gallstones. Because of these risks, lifelong follow‑up and daily vitamin supplementation are essential.
Important: Bariatric surgery is a powerful tool, but it isn’t a cure. Success depends on your commitment to dietary changes, regular exercise and mental health support.
Recovery and long‑term commitment
Expect to spend 1–2 days in the hospital and take several weeks to return to normal activities. Your diet will progress in stages: liquids, puréed foods, soft foods and finally solid foods over the course of six to eight weeks. Regular check‑ups with your surgeon and dietitian ensure you’re healing well and getting enough nutrients.
After surgery, you’ll need to:
- Eat mindfully: Focus on high‑protein foods, chew thoroughly, avoid sugary and high‑fat items and never drink liquids with meals.
- Take vitamins: Lifelong supplementation prevents deficiencies in vitamins B₁₂, D, iron and calcium.
- Move your body: Gentle walking begins soon after surgery. Gradually incorporate cardio and strength training as your doctor recommends.
- Stay connected: Attend follow‑up appointments, join support groups and work with mental health professionals to address emotional eating and body‑image changes.
Conclusion
Bariatric surgery can be a life‑changing tool for people struggling with severe obesity. It leads to substantial weight loss and health improvements, but it requires careful preparation, informed decision‑making and a lifelong commitment to healthy habits. At Novara Academy, our programs Pre‑Op, Life After and Evolve provide the education, coaching and community you need to navigate every stage of the journey. If you’re considering surgery, start by consulting with a bariatric specialist and exploring the resources we offer.

